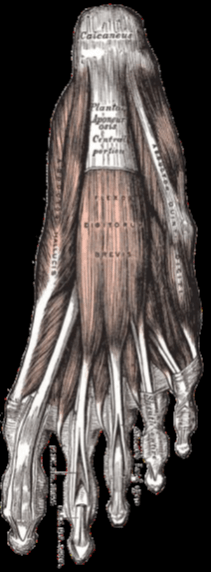
 An estimated ten percent of the general population develops heel pain at some point in their lives, and many of these people present this complaint to their general practitioner. Plantar fasciosis is the most common source of that pain. More traditionally, the diagnosis has been termed “plantar fasciitis.” However an evolving understanding of this condition demonstrates that this problem is not an inflammatory response – deemphasising the usefulness of inflammation-oriented treatment protocols. Histopathologic studies show that patients with a plantar fasciitis diagnosis have more disorganization of fibrous tissue similar to degenerative tendinosis rather than inflammation. This new understanding leads to an emphasis on first-line treatments that modify the variables known to lead to additional stress on the attachment of the plantar fascia to the calcaneus.
An estimated ten percent of the general population develops heel pain at some point in their lives, and many of these people present this complaint to their general practitioner. Plantar fasciosis is the most common source of that pain. More traditionally, the diagnosis has been termed “plantar fasciitis.” However an evolving understanding of this condition demonstrates that this problem is not an inflammatory response – deemphasising the usefulness of inflammation-oriented treatment protocols. Histopathologic studies show that patients with a plantar fasciitis diagnosis have more disorganization of fibrous tissue similar to degenerative tendinosis rather than inflammation. This new understanding leads to an emphasis on first-line treatments that modify the variables known to lead to additional stress on the attachment of the plantar fascia to the calcaneus.
Another subject of evolution in this diagnosis is the utility of a wait-and-see approach to the initial complaint. In many cases, the patient has independently attempted a wait-and-see approach for months before contacting his or her general practitioner about plantar fasciosis. Wolgin and colleagues found that patients experiencing plantar heel pain wait an average of eight months before seeking medical attention. Sports physician John Orchard discusses the modern imperative of keeping patients active for general health, how plantar fasciosis works as an impediment to healthy activity, and how this underscores the importance of quick, lasting, and meaningful attenuation of symptoms.
Given these understandings, first-line treatment of plantar fasciosis may include:
Flexibility Improvements: Patients with an ankle dorsiflexion range of less than ten degrees demonstrate twice the likelihood of developing plantar fasciosis. Supervised stretching, home exercise plans, manual therapy, and nocturnal splints have all been demonstrated to produce both short and long-term improvements for patients managing plantar fasciosis.
Strengthening: Targeted, strategic muscle strengthening programs have been shown to improve force attenuation.
Pedal Biomechanical Supports: This generally involves shoe consultation, taping, and orthotic assessment. Patients should be counselled on optimal shoe choices, recognizing the need for shoe replacement, and shoe rotation during the work week. For people who work on their feet, during-the-week shoe rotation has been shown to reduce the risk of plantar fasciosis.