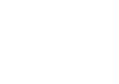Physical Therapy Billing Software
Apollo Practice Management includes Physical therapy billing software that puts you in complete control of all your billing requirements. Our software service eliminates the cost of maintaining traditional medical billing processes and resources in order to maximize profits. From private bills, insurance claims, bulk billing and employee payments, all invoice requirements can be created and dispatched directly to the patient seamlessly. Apollo Practice Management enables you to clearly code each bill to accurately reflect the purpose and minimize confusion and financial losses.
Patient Invoicing
Apollo Practice Management includes automating all your invoicing needs for patients using simple templates adapted to your individual need. Using the automated physical therapy billing services, you can then send the invoice directly to the patient, employers, Insurance companies, or bulk bill, or keep it saved as a PDF for your patient records.
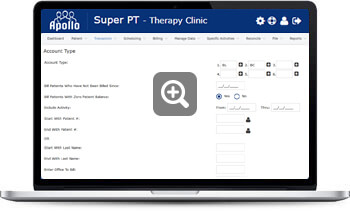
Insurance Claims
Our software is designed to pay your claims faster with minimal rejection in order to maximize your compensation. It helps clinic staff to track billable amounts, unpaid claims and receivables more efficiently and effectively. Our Physical therapy billing software will immediately notify you by email whether the claim is approved or rejected.
Insurance Payments
Apollo is fully 5010 compliant. Included within this module is an 835 and 837 format which allows you to e-post payments. Earlier without the automatic PT billing software Medicare Payment tasks would take you all day to put in details, but now it just a matter of minutes.
New Rule Identification
As Apollo Practice Management is based on SAAS application our clients are always up to date with latest insurance claim news. No need to check on updating new rules for claim applications, we do it all for you to ensure your claims are received and accepted.
Cash pay and overpay
More and more clinics are going to cash pay. This walkout receipt allows the patient to turn it into their payer (whether Insurance, HSA, or other payer) and be paid. In addition to this, we have an overpay feature in the walkout receipt so that if the patient decides to give you more than 1 visit worth of payment, you can put the rest in overpay. The overpay will be reflected in the patient transactions.
Inbuilt optimization of your bills by tracking payor CAP
Apollo tracks allowed amounts from payors and makes it simple for you to optimize revenue receivables, simply enter the KX modifiers and Apollo will keep track of the CPT codes by allowed charge. Once the expected/allowed amount reaches the limit, it will put a KX modifier to the CPT code and saves you guessing at CAP amounts.
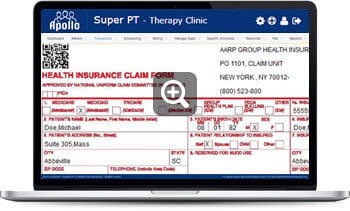
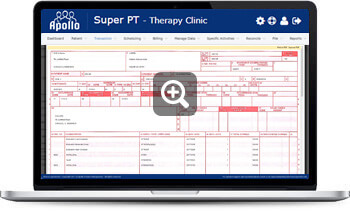
Full support for UB-04 Form
The UB-04 is the red-ink on white paper standard claim form used by institutional providers for claim billing. Although it was developed by The Centers for Medicare and Medicaid (CMS), it has become the standard form used by all insurance carriers. Who can bill claims using the UB-04? Any institutional provider can use the UB-04 for billing medical claims. The following is a partial list Community Mental Health Center, Comprehensive Outpatient Rehabilitation Facility, Critical Access Hospital, End-Stage Renal Disease Facility, Federally Qualified Health Center, Histocompatibility Laboratory, Home Health Agency, Hospice, Hospital, Indian Health Services Facility, Organ Procurement Organization, Outpatient Physical Therapy Services, Occupational Therapy Services, Speech Pathology Services, Religious Non-Medical Health Care Institution, Rural Health Clinic, Skilled Nursing Facility.
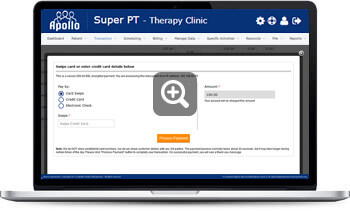
Seamless credit card processing
Apollo partners with BluePay a premier integrated payment provider. Credit card processing can be used for all types of transactions. A simple guided setup helps our Physical therapy practices start processing credit cards using an encrypted card scanning system. Competitive transaction processing rates with modern technology make BluePay the partner of choice for credit card processing.
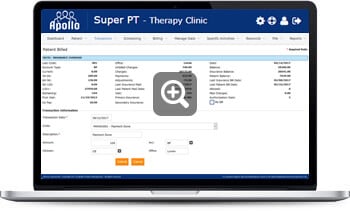
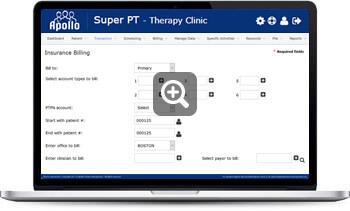
Insurance Billing by Payor
This will allow Apollo users, even if they predominantly use Account Categories to bill, to bill per payer (Insurance Company). We have several clinics that may have a problem with one particular payer and prefer to bill by payer because of certain circumstances. When going to Insurance Billing by Account Type, you will be allowed to leave account type blank and bill the payer.